Our research shows that higher Bone Mineral Density (BMD) was associated with a greater risk of fracture, which is opposite of what we would expect. When we picked apart the BMD ratio we found that bone size had the strongest association with fracture risk, such that smaller bones had a greater risk.
The 2023 Health Summit will share new pathways for translating knowledge into practice for the Implementation of early detection and intervention for cerebral palsy from the best researchers and clinicians in the field.

This study tested the safety and effectiveness of a neuroscience-based, multi-component intervention designed to improve motor skills and sensory processing of the more-affected arm and hand in infants with CP where one side is more impacted than the other (asymmetric CP).
Dr. Nathalie Maitre discusses the CPF Early Detection and Intervention Network and helps us to understand how babies learn, how CP impacts the developing brain, and early intervention strategies that can help.

CPF Executive Director Rachel Byrne and Christina Smallwood talk about parenting, raising a child with cerebral palsy and helping her learn to advocate for herself.

CPF Executive Director Rachel Byrne and Dr. Mary Lauren Neel, MD discuss Life after the NICU.

Good nutrition is critical for your child's healthy brain development. It's not uncommon for families to struggle getting enough food to eat. If you feel like you haven't had enough food to feed your whole family in the last month, please talk to someone. This is a common problem.

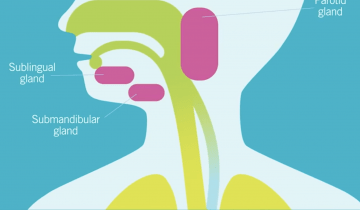
Drooling is an important problem for many individuals with CP and there are a number of interventions available to treat symptoms. If an individual with CP or their caregiver have concerns about drooling it is important to discuss with a health care provider. Care pathways such as the AACPDM pathway can be a starting point for shared decision making. In all cases, working together as a team is important in choosing the best alternative. Children and adults with CP may have trouble with drooling, or saliva management. In the medical world, drooling is referred to as sialorrhea. Saliva plays an important role in eating but also can interfere with airway clearance and breathing, as well as social participation. When drooling has this kind of impact it becomes important to consider intervention.
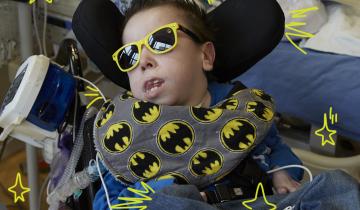
My boys were exactly the same amazing, lovable, adorable, brilliant little boys after the diagnosis, that they had been before it. The exact same.

Many children with cerebral palsy (CP) have difficulty controlling saliva. Drooling varies in severity and can be distressing for the children, families and caregivers. Chronic drooling is referred to as Sialorrhea and occurs as a result of limitations in a person’s ability to control and swallow oral secretions.
Neuroplasticity is the ability that the brain has to form new connections between different cells or between different areas of the brain.

Oropharyngeal dysphagia, or OPD, is an impairment of the oral or pharyngeal phases of the swallow. This can impair muscle movements and coordination of the mouth, such as the lips, tongue, jaw, cheeks, palate, and also muscles of the pharynx and the entry to the airway.

The typical cognitive assessments that are used for children require them to be able to use their hands to point to pictures or hold puzzle pieces.

Cerebral palsy is caused by damage to the infant brain. This damage can involve not only the motor parts of the brain, but also the parts that deal with vision. This is not related to damage to the eye but is related to damage of the parts of the brain that process visual information.

Weight, height and body composition are important indicators for development. The tools used to measure these can be different for children with cerebral palsy.

Children with cerebral palsy (CP) often grow poorly and assessment of growth in this population is further complicated by two main difficulties. Firstly, children may have joint contractures, muscular weakness, scoliosis, and/or involuntary movements that make standing or lying straight difficult, if not impossible.
When we have a physical disability, our bones can get a bit weak or osteoporotic. Something that can be improved is promoting bone health for people with cerebral palsy.

As a parent, when it comes to different types of interventions for infants with cerebral palsy, how do you know what you have, what you don't, and what you could get?

Exploration for an infant means discovering anything about that environment. If that infant needs an opportunity to be brought to them, that's okay. Let an infant explore through their senses, whether it's touch, or smell, or taste, or sight, or hearing.

Cerebral palsy is an injury to the brain, but what we find is that it has a lot of effects on how you use your muscles.

"Cerebral palsy is primarily a motor impairment so it's really important to look at what the child’s motor function is. Are they developing on the trajectory of a child who has cerebral palsy or are they developing as we would expect a baby to develop? "
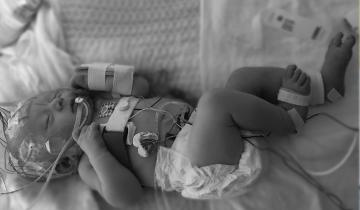
For a child with CP learning to move, the really important things to remember are that the child should always be active.

Babies develop about 80% of their brain growth over the first two years of life, and it's also when all the connections in the brain, what we call the white matter, which is the cables in the brain, grow and develop and connect to the cortex.
Receiving early diagnoses or high‐risk for CP classification is a parent priority. Alignment between parents and providers exists for International Classification of Function domains of body functions/structures and activity, but less for those of environment, personal, and participation.

