How important is it to control drooling and other frequently asked questions
Drooling is an important problem for many individuals with CP and there are a number of interventions available to treat symptoms. If an individual with CP or their caregiver have concerns about drooling it is important to discuss with a health care provider. Care pathways such as the AACPDM pathway can be a starting point for shared decision making. In all cases, working together as a team is important in choosing the best alternative.
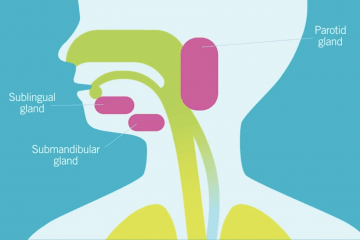
Children and adults with CP may have trouble with drooling, or saliva management. In the medical world, drooling is referred to as sialorrhea. Saliva plays an important role in eating but also can interfere with airway clearance and breathing, as well as social participation. When drooling has this kind of impact it becomes important to consider intervention.
How important is it to control drooling?
This is a decision that individuals with CP, caregivers and clinicians navigate together. If saliva is not causing any problems, the decision may be to simply monitor.
When would an intervention be considered?
If a child’s chin is frequently irritated or infected, if the presence of drool is causing social complications, damaging things in the environment like schoolwork or a computer, or affecting a child’s self-esteem there may be motivation to treat. Clinicians often guide individuals or families more strongly towards treatment if there are repeated respiratory symptoms or infections as these may lead to more serious consequences.
What treatment options are available?
Choosing a treatment option is tailored to an individual’s needs and starts with a thorough review of the history. Sometimes a treatable cause for drooling is identified, such as a tooth abscess or untreated gastroesophageal reflux. Other times a medication which has a side effect of drooling is identified and an adjustment can be considered. If the decision is made to “do something” about the drooling the intervention chosen is usually the least invasive choice that appears appropriate for the situation. For example, a six year old who is motivated to manage their drooling may benefit from a behavioral approach, with tools to remind then to swallow or wipe away their saliva.
When are medications used to control drooling and what are they?
Oftentimes a pharmacologic (medication) approach to drooling treatment is necessary. Perhaps there is some urgency in treating the symptoms. Or perhaps behavioral or oromotor methods are not effective or appropriate. When this is the case there are a number of medications available which can help to reduce saliva. Currently, only one medication, glycopyrrolate, has been FDA approved for the specific purpose of treating drooling in children. There are others which may be considered, such as a scopolamine patch and atropine drops applied under the tongue, but their use is off label (meaning the medicines are approved for use in children for other purposes, but not drooling). All of the medications used for drooling continue to be studied for effectiveness, both alone and in comparison to one another. Regardless of the medication chosen, close communication between the individual taking the medication and the clinician prescribing it is important. Quite often little adjustments in dosing are necessary. Equally important is monitoring for side effects of the medication.
What if medication doesn’t work?
If multiple medications have been tried and are either ineffective or have intolerable side effects it may be time to consider more invasive treatments. Salivary gland injection with botulinum toxin can be very effective and generally has few side effects which impact the whole body. The drawbacks are that it often requires general anesthesia and needs to be repeated regularly because effect wears off after several months. You can learn more about botulinum toxin injections here.
What surgical options are available?
The most definitive (and most invasive) drooling treatment option is surgery. This is generally directed towards ligation (clipping) or re-routing some of the salivary ducts, or removing salivary glands entirely. The nuances of which type of surgery is appropriate vary from individual to individual. Surgeries are also not without side effects, although they are generally well tolerated, and the decision to pursue surgical intervention is one that is arrived at when treatment is a priority and other alternatives have either been ineffective or are not feasible.
To Learn More
Choosing a treatment option is tailored to an individual’s needs and starts with a thorough review of the history. This is a decision that individuals with CP, caregivers and clinicians navigate together.