The GMFCS can be a helpful tool in clinical and research use and has been shown to be stable and accurate over time. It can also help individuals and families better understand cerebral palsy.
Though the initial insult or injury to the brain that causes cerebral palsy is non-progressive, aging with cerebral palsy and lack of physical activity during critical periods of development can impact biologic and metabolic function for adults with cerebral palsy.
We got the diagnosis of Cerebral Palsy when Lelia was 18 months. I was really happy, as we didn’t know what was wrong with her before then. She had low tone. She couldn’t roll over. She couldn’t sit up. Of course she didn’t walk. The diagnosis gave it a name, something I could work with, and I became a kind of vigilante mother, determined to get the best care for my daughter.

There are multiple factors that impact bone health, including birth weight, nutrition, medications for seizures and/or reflux, genetics, and physical activity. Targeted exercise to improve bone health in childhood can be sustained into adulthood, and childhood is the best time to promote bone health.
As we all know, becoming a teenager means significant upheaval, not only physically, but in terms of friendships, in terms of learning, and life outlook. This is also true for adolescents with cerebral palsy and other developmental disabilities. We know that whilst we may of spent a lot of time focusing on their physical abilities and other difficulties it is not the only part of their life.

Around the age of six all children are going off to school. Children move from explorative play, which is fairly informal to a much more formal day. That can be a lengthy day and it's quite structured. There are a lot of challenges faced by children with cerebral palsy throughout the school year.

Weight, height and body composition are important indicators for development. The tools used to measure these can be different for children with cerebral palsy.

Children with cerebral palsy (CP) often grow poorly and assessment of growth in this population is further complicated by two main difficulties. Firstly, children may have joint contractures, muscular weakness, scoliosis, and/or involuntary movements that make standing or lying straight difficult, if not impossible.
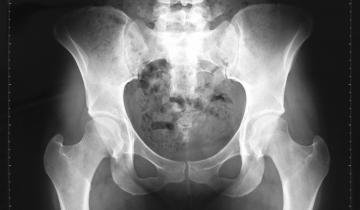
When treating a child with CP, part of a pediatrician’s job is assessing and treating children with abnormal tone difficulties, as well as other muscular-skeletal problems. From around the age of two years, kids start to develop difficulties with muscle tone that can have an impact on their hip development.

