An update to the current understanding and potential of stem cell therapies for CP.
Intervention to improve function for children and young people with cerebral palsy needs to include client-chosen goals and whole-task practice of goals. Clinicians should consider child/family preferences, age, and ability when selecting specific interventions.
We studied how common pain was thought to be due to muscle spasticity in the legs or arms is in children/adolescents with CP.
Drooling is an important problem for many individuals with CP and there are a number of interventions available to treat symptoms. If an individual with CP or their caregiver have concerns about drooling it is important to discuss with a health care provider. Care pathways such as the AACPDM pathway can be a starting point for shared decision making. In all cases, working together as a team is important in choosing the best alternative. Children and adults with CP may have trouble with drooling, or saliva management. In the medical world, drooling is referred to as sialorrhea. Saliva plays an important role in eating but also can interfere with airway clearance and breathing, as well as social participation. When drooling has this kind of impact it becomes important to consider intervention.
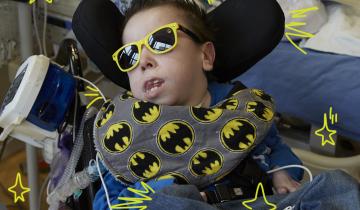
Our 3rd Virtual Town Hall featured experts from the Shirley Ryan Ability Lab and Northwestern University in Chicago. This multi-disciplinary panel discussion highlights the latest updates in care of children with #CerebralPalsy.

Purpose of review: Cerebral palsy is the most common physical disability of childhood, but the rate is falling, and severity is lessening. We conducted a systematic overview of best available evidence (2012-2019), appraising evidence using GRADE and the Evidence Alert Traffic Light System and then aggregated the new findings with our previous 2013 findings. This article summarizes the best available evidence interventions for preventing and managing cerebral palsy in 2019.
It is recommended that women start having mammography screenings starting at about the age of 40, and it becomes more difficult to obtain these services if you have a disability.

The findings of this article demonstrate the need for improved screening rates in women with CP, and highlight areas for improving their screening experience.
When first meeting a parent who's had a child newly diagnosed with cerebral palsy, I really want to try and help them understand their baby. It can be difficult for parents to take it in all at once and many leave that first interview quite overwhelmed, but you're going to meet some really important and helpful people.

Babies develop about 80% of their brain growth over the first two years of life, and it's also when all the connections in the brain, what we call the white matter, which is the cables in the brain, grow and develop and connect to the cortex.
Spasticity is a condition of muscles that is a velocity resistance to stretch. What that means to a child and to a parent is that if you move the limb slowly, you have a difference than if you move that limb fast. Spasticity restricts movement and it creates a break on the system. It's as if they're trying to move, but they're held back. By treating spasticity, you may improve the range of motion or the action of the movement.

Sleep is important to all of us, but it's especially important for infants. When infants go to sleep, they start to create neural networks about what they've been learning during the day. It's estimated that as many as one in five children with disabilities have a sleep disorder, and that's higher than the rate of typically-developing children. Finding sleep interventions for these children is incredibly important so they can lay down their brain networks and continue to learn during their early childhood years.

A lot of parents don't realize that their baby, all the skills that they have. So they can look at you, they can follow you. They're already starting to imitate you, and through the first few months of life, they're already starting to learn to reach and grasp toys, and to have nonverbal communication with you.

Early diagnosis begins with a medical history and involves using neuroimaging, standardized neurological, and standardized motor assessments that indicate congruent abnormal findings indicative of cerebral palsy. Clinicians should understand the importance of prompt referral to diagnostic-specific early intervention to optimize infant motor and cognitive plasticity, prevent secondary complications, and enhance caregiver well-being.
